AI-Driven Automation Tools
Resupply, Rental, and POS Workflows
Delivery Management and Mobile App
Hello, AI — Full-Cycle Revenue Automation
Instantly verify patient insurance coverage, benefits, and deductibles in real time before the order is placed. Seva AI automates prior authorization requests with payer-specific rule engines — reducing approval time by 60% and eliminating late-stage claim rejections caused by eligibility gaps.

Seva AI pre-scrubs every claim before submission — checking for coding errors, missing modifiers, incorrect HCPCS codes, and compliance flags. Our intelligent claim engine delivers a 97%+ clean claim rate across Medicare, Medicaid, and commercial payers. Claims are submitted electronically with full 837P/837I support.

AI-powered denial detection identifies root causes automatically and generates appeal letters with one click. Seva AI learns payer-specific denial patterns from your claim history and proactively prevents repeat denials — reducing your overall denial rate by up to 40%.

Automatic ERA/EOB posting, payment reconciliation, and secondary billing — all matched in real time to open claims. Patient-friendly statements and an online payment portal close the revenue cycle loop with a seamless financial experience for your patients.

Real-time dashboards tracking AR aging, collection rates, denial trends, payer performance, and revenue projections. Seva AI provides predictive revenue forecasting so you can anticipate cash flow and make proactive business decisions with confidence.

Since switching to Pracura Tech RCM, our denial rate dropped by 38% and our AR days went from 45 to just 14. The Seva AI claim scrubbing alone pays for itself every month.
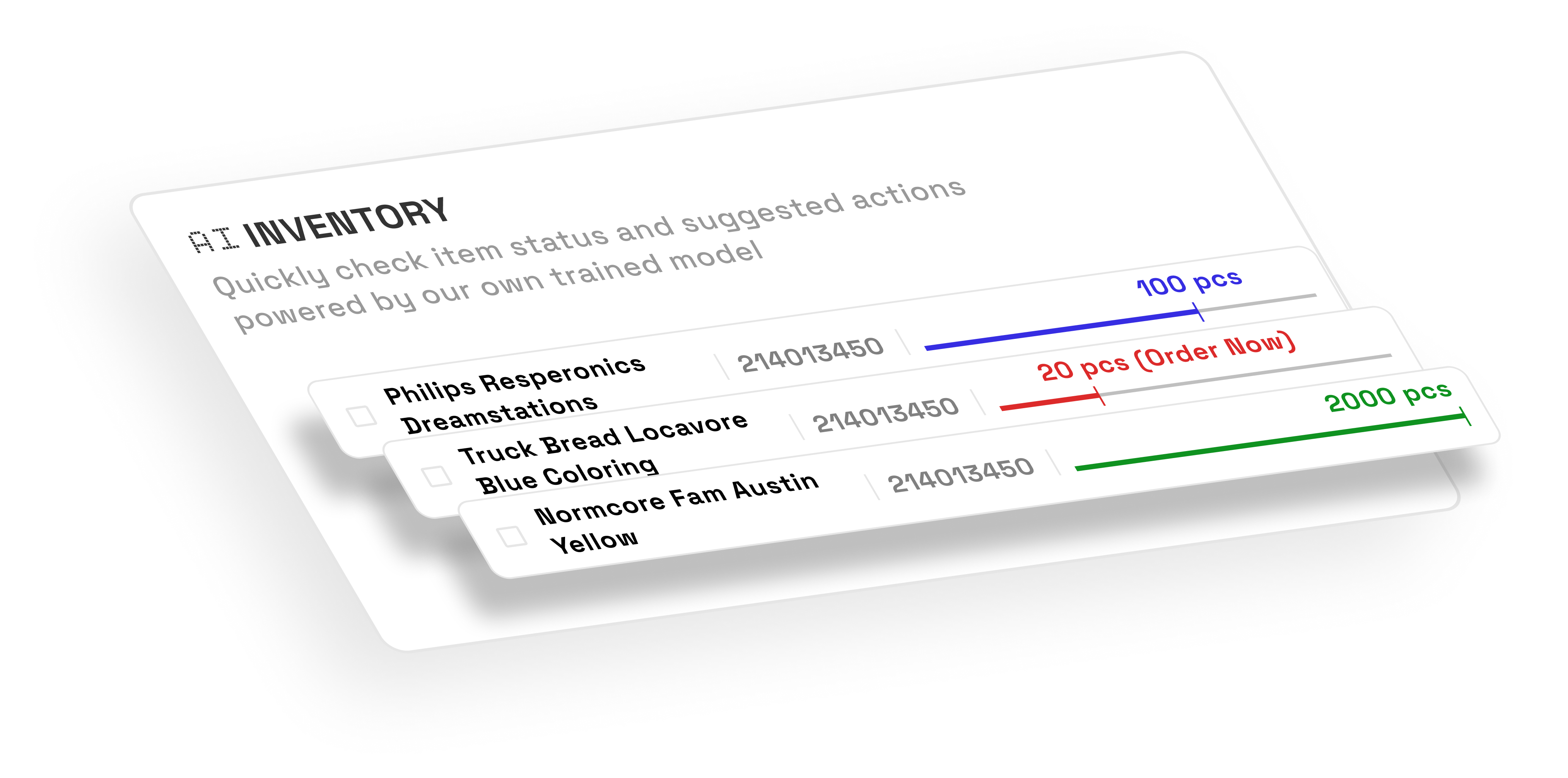

Stop forcing your team to work around outdated software. Our end-to-end platform is built to mirror your specific HME workflow—from the first referral intake to the final collection.